By Erinn Aspinall

Female skeleton model at the Bio-Medical Library.
We just purchased our first female skeleton model at the Bio-Medical Library. This purchase might seem a long time coming — that in 2018 our anatomy collections should already have broad representation.
But the story of our first female skeleton is a complex one that can be traced back as early as the 1500s and continues today in contemporary anatomy texts and teaching tools.
The ‘male standard’
A long history of research has shown that medical education texts typically default to the male standard — with males represented in case studies and anatomical drawings, and depictions of females mostly limited to examples of reproductive anatomy.
“It was surprisingly hard to find a female skeleton model,” said Collections Coordinator Nicole Theis-Mahon. She explained that the source she used for purchasing a female skeleton model offered a pelvis, a pelvis with female genital organs or pelvic floor muscles, or a childbirth demonstration model.
“Not only were the female models disembodied, but the few full skeletons were also more expensive than their male counterparts,” added Theis-Mahon. This means that information available to libraries, educators, and students can be limited. It means that the learning that takes place through anatomical comparisons is lost.
Trend dates back to the 1500s
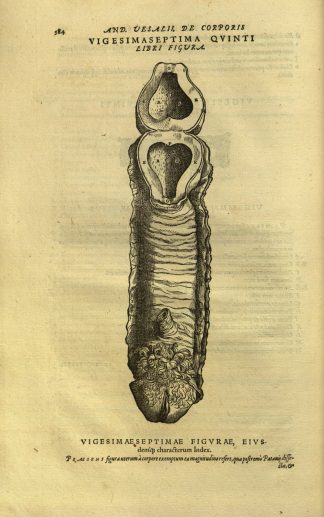
Illustration of female reproductive system from De Humani Corporis Fabrica by Andreus Vesalius (1543).
The male standard in anatomy is not new. Evidence of this approach can be traced back to the times of Andreus Vesalius — who is known as the founder of modern human anatomy.
In his landmark work De humani corporis fabrica (1543), Vesalius offered an imagined version of the female reproductive system that highlighted its homologies with the male reproductive organ, rather than displaying what is today understood as an entirely different set of organs.
Cultural origins
“In addition to theoretical rationales, the limited depiction of the female form in early anatomical texts was also cultural,” says Emily Beck, Assistant Curator of the Wangensteen Historical Library of Biology and Medicine.
“Dissections for research and learning happened much less frequently in the early modern period than they do today,” said Beck. “The cadavers used in early dissection were condemned criminals. Women were infrequently represented this population, so they were dissected less often.”
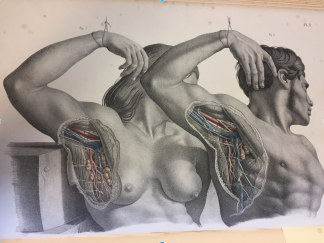
Male and female lymph node dissection from Surgical Anatomy by Joseph Maclise (1851).
Moving forward to 1851, we are able to share the one example from our Wangensteen Historical Library that depicts a side by side anatomical comparison of a male and female that is not tied to reproductive anatomy.
This example comes from Joseph Maclise’s Surgical anatomy (1851) and illustrates the lymphatic system. Although there is a direct comparison made between the male and female anatomy, it is noteworthy that the male subject’s arm obscures the female subject’s face, anonymizing her.
The ‘hidden curriculum’ in contemporary anatomy texts
A 2017 study by Parker et al. on the visual analysis of gender bias in contemporary anatomy texts reflects on previous research studies from 1986 to 1998, and completes a present-day analysis of anatomy texts that are currently used in health professional curricula.
The researchers found that the representation of the human form in anatomy textbooks remains predominantly male, except within the sections about reproductive anatomy. Moreover, the researchers found that in comparison to studies conducted over two decades ago, the representation of females in anatomy textbooks has only improved by four percentage points.
They found that underrepresentation within anatomy texts was also evident across a broader representation of sex (male, female, intersex), ethnicity, age, body type, and health status — with the white, young, healthy, muscular male set as the standard model.
Morgan et al. (2014) refer to the male standard in anatomy textbooks as a “hidden curriculum” as it “implies outcomes that are learned, but are not intended.” And “includes beliefs, values, and norms taken from the classroom experience and applied beyond the classroom.”
Impact of the male standard
Research shows that gender bias continues in the practice of medicine — as gender stereotypes have impacted diagnosis, treatment, and management of patients. So, it’s important that the students who will become our future health providers get a broader understanding of human anatomy than what currently exists in textbooks.
Sex-based differences in anatomy can affect patient outcomes and are critically important for future practitioners to learn. It is also vital for future health providers not to equate biological sex characteristics with gender identity.
“The majority of people with female bodies will have a female gender identity, however their gender identity does not always match their anatomical bodies or secondary sex characteristics,” said Eli Coleman, Director of the U of M Program in Human Sexuality. “There is a diversity of gender identities and gender role expressions that are determined by other complex factors.”
Addressing gender stereotypes
Our University Libraries provides information and tools that support students and educators. But what happens when the information we would like to share simply does not exist or is otherwise inaccessible?
For a start, we can buy a female skeleton model for our students.
We can also supplement textbooks with other student learning experiences.
The University’s Program in Human Anatomy ensures that students are able to learn equally about male and female anatomy.
“Our anatomy students have the opportunity to learn from donors through our Anatomy Bequest Program,” said Tony Weinhaus, Ph.D., Program Co-Director.
“Males and females have equal representation in the program,” adds Weinhaus. “It is through this experience that anatomy students can develop a representative and holistic understanding of the human form that mirrors what they will experience when they become practitioners.”
And we can use the limitations of available information as an opportunity to start a conversation.
“When I work with the gross anatomy students in the Medical School, I share historical images from Veslius and Maclise to help students begin to learn that active recognition of gender bias should be part of their daily routine as healthcare practitioners,” said Beck.
“Developing this mindset reinforces the practice of critical evaluation that can help reduce the impact of the gender bias that is so prevalent across medicine.”